Millions of employees rely on ALEX each year to help them navigate their benefits options so they can pick the right plan for them and their families. But sometimes employees also want the plan to include the doctors they already visit.
In fact, our research shows that 93% of likely ALEX users agreed they would need to be able to verify their provider is in-network in order to make a confident decision about their health plan.
That’s why we added a provider search feature to ALEX—powered by Ribbon Health—so your employees can easily see if a specific healthcare provider is in-network when they pick their medical plan. By having this information at their fingertips, employees can use this information to make wallet-friendlier choices by staying in-network.
This means employees can check for in-network providers and compare different providers—even across carriers—all within ALEX. What’s more, Ribbon Health’s extensive provider and network data includes 99% of providers in the U.S.
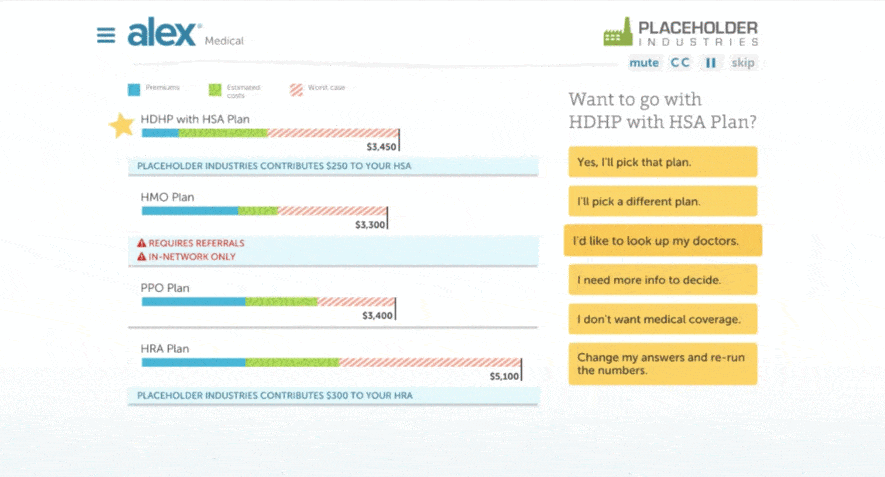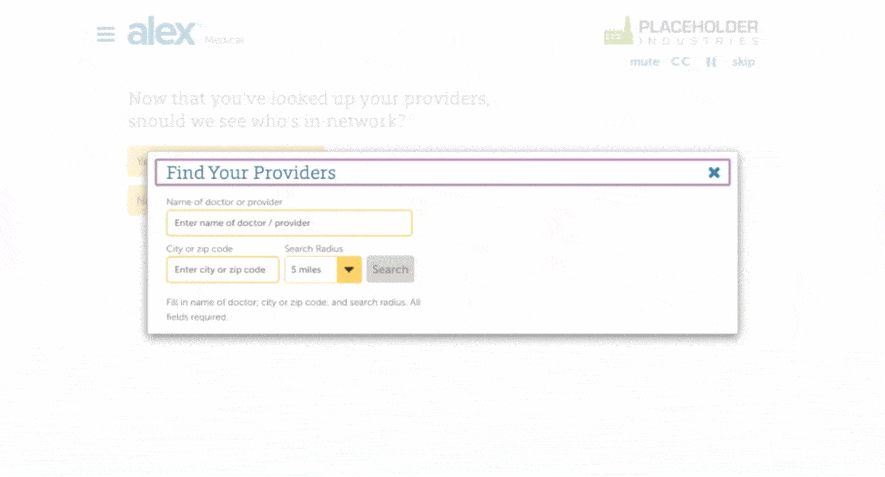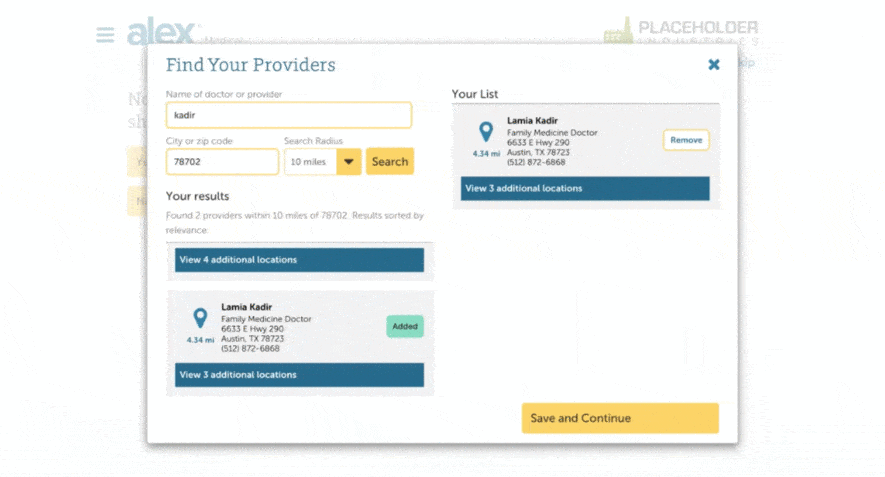
Enabling your employees to see which providers are in-network, before they pick their plan allows you to:
✅ Avoid costly out-of-network visits for employees and your organization.
✅ Help employees feel confident about both coverage and cost.
✅ Give employees the assurance they need to change plans.
✅ Reduce medical plan buyer’s remorse.
At Jellyvision, we’re on a mission to help you turn your workforce into smart healthcare consumers, and mitigating out-of-network costs is just one of the ways in which we’ve set out to do that. Be on the lookout for more ALEX features to help you and your employees spend less on health care.


