Choosing between buying food and necessary prescription medicine: this isn’t a decision that anyone should have to make. But for many Americans, this is their current reality.
A recent study from Gallup and West Health showed that 14% of U.S. adults couldn’t pay for their medications, while 30% skipped treatment because of the cost of care.
Even higher-income households that earn more than $120,000 per year are affected by the astronomical cost of healthcare: 20% admitted that cost is a reason they wouldn’t seek care.
There’s substance behind their concerns. A study by Credit Karma of its members showed that its 22.6 million members hold $48.6 billion in medical debt — that’s more than $2,000 per member. With medical costs expected to grow by 7.6% in 2022, this problem isn’t just going to go away.
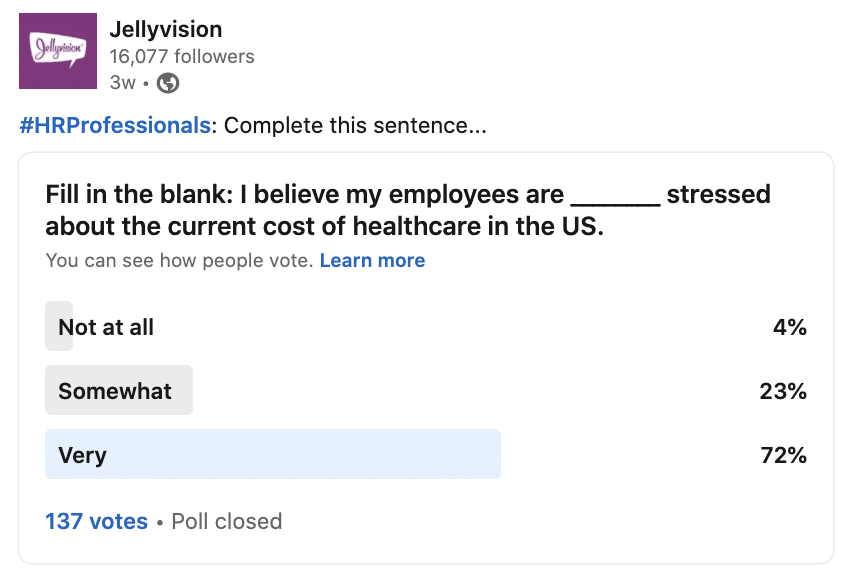
Do healthcare costs affect our employees’ mental health and stress levels?
Short answer? Yes. Of course.
Even before the pandemic, two-thirds of Americans said the cost of health insurance was a stressor, whether for themselves, their loved ones, or in general, according to the 2018 Stress in America: Uncertainty About Health Care report. Stress was high regardless of income level: 64% of those with an annual household income of under $50,000 cited health insurance costs as a source of stress, compared to 69% of Americans who earn $50,000 or more.
Chronic stress over healthcare costs can have significant health consequences for employees — particularly for their mental health. But when these issues arise, not all employers offer access to appropriate resources. The lack of access to mental healthcare is an additional source of stress, primarily for younger generations like Millennials (56%) and Gen Xers (47%).
This is a problem, because since the pandemic, over 40% of Americans have reported an increase in mental distress. According to the National Alliance on Mental Illness, in 2020, 1 in 5 adults experienced mental illness, and 1 in 20 experienced serious mental illness. Yet less than half (46.2%) of American adults with mental illness were treated.
When left untreated, mental illness leads to physical health problems. For example, people suffering from depression have a 40% higher risk of developing cardiovascular and metabolic diseases. And nearly a third of adults with mental illness also had a substance abuse disorder in 2020.“Mental health and addiction recovery services will likely be of greater need in the coming year. The pandemic has been a prolonged, traumatic event that has caused isolation, fear and anxiety for some of the workforce. Providing recovery support services as well as a safe space for employees to use it will help avoid stress and other related health concerns that can have significant long-term impact to the employee and the workplace.”

This mental distress plays out in a variety of costly ways in the workplace. Employees with mental health issues are more likely to miss work. Employers lose an average of $4,783 per year per employee for lost days. Depression alone costs employers an estimated $44 billion yearly in lost productivity.
Stressed employees are also more likely to quit their job, raising turnover and replacement costs. Losing an employee costs an employer, on average, $5,733 per year per employee.
Finally, employees suffering from mental distress are more likely to use healthcare services. On average, they use $3,000 more in services per year than their peers.
Employees shouldn’t have to resort to crowdfunding to pay for their medical bills, and they shouldn’t skip treatment because they’re worried about whether they can afford it. This is where employers like you can make a difference.
This mental distress plays out in a variety of costly ways in the workplace. Employees with mental health issues are more likely to miss work. Employers lose an average of $4,783 per year per employee for lost days. Depression alone costs employers an estimated $44 billion yearly in lost productivity.
Stressed employees are also more likely to quit their job, raising turnover and replacement costs. Losing an employee costs an employer, on average, $5,733 per year per employee.
Finally, employees suffering from mental distress are more likely to use healthcare services. On average, they use $3,000 more in services per year than their peers.
Employees shouldn’t have to resort to crowdfunding to pay for their medical bills, and they shouldn’t skip treatment because they’re worried about whether they can afford it. This is where employers like you can make a difference.
Where employers are still falling short when it comes to mental health
Although 32% of employers have invested in mental health resources, another 28% were unsure about taking action or weren’t taking action at all regarding their employees’ mental health, according to a McKinsey study.
If your company is among those that have not yet taken action to support employees’ mental health, you may want to change that soon. Nearly all (95%) of HR professionals in our recent survey anticipated that in the future, employees will continue to seek mental health care at a higher rate than they did before the pandemic, and two-thirds of employees agreed.
Even if you’re among the employers that are trying to support your employees’ mental health, your implementation and communication strategies may have fallen short. Our research found a number of disconnects between what HR thinks they’re doing to support their team members and how employees actually perceive those efforts:
When we asked employees about why they aren’t using their mental health benefits, many mentioned that they don’t know what benefits are available and don’t understand their options. But the number-one problem they cited was the cost. After all, when employees think about selecting their benefits, the first thing they think about is the price. Combine that worry with the stress that 52% of employees feel when choosing a health plan, plus financial concerns in the wake of COVID-19, and it’s a perfect storm for bad decisions.
How employers can address their employees’ stress
Fortunately, employers can eliminate some of the friction and stress from the open enrollment process. If you follow these three steps, you’ll show your employees how to save on their healthcare expenses and help them make smarter healthcare decisions.
1. Break down your employees’ potential savings with health savings accounts (HSAs).
A third of employees with an HSA available never open their accounts. And the average employee contribution, $1,949, doesn’t cover most employees’ out-of-pocket medical expenses. That’s often because employees don’t fully appreciate the benefits of their HSA.
Explain to employees that their HSA contributions are pre-tax and illustrate how much they could wind up saving — and avoid sending to the IRS — by investing in an HSA.
It’s also important for your employees to know that they can use their HSA to save for retirement. Much like a retirement savings account, HSAs can be invested and grow year after year. Be sure to explain how much, in tangible numbers, how much your employees can earn in interest. Don’t forget to mention this benefit: after your employees turn 65, they can spend their HSA savings on nonmedical expenses.
2. Reframe HSA messaging about contributions as monthly rather than yearly.
The ultimate goal is for your employees to max out their HSAs so they can cover their out-of-pocket medical expenses. But if you’re communicating their potential contribution as a yearly lump sum rather than as a per-paycheck contribution, it may seem overwhelming.
Psychologically, it’s a lot easier for most employees to part with $156 per paycheck than to part with $4,000 all at once. So talk to your employees about what the average employee contributes per paycheck and, if you want to share a yearly amount, focus them on the amount they’ll potentially save in taxes.
3. Make it easy for employees to make better decisions with a benefits engagement tool.
Employees often choose the same plan year after year, but that’s because it’s the path of least resistance. And it may seem daunting or inconvenient to hunt down someone from HR to answer questions — especially if your employees don’t know what questions to ask. (Plus, your HR team probably doesn’t have time in their day to offer one-on-one consultations with all of your employees.)
That’s where a 24/7 benefits savings and guidance tool, like ALEX, comes in. ALEX asks questions that help it deliver personalized recommendations in plain language to ensure employees understand their benefits. Best of all, ALEX’s advice is tailored to each employee’s situation — including their health, financial, and life circumstances, plus their priorities and goals.
Employees who use technology like ALEX say they better understand their benefits options. And employees who use ALEX put 36% more into their HSAs than the national average.
While we admit that having a conversation with ALEX may not be quite as relaxing as sipping your beverage of choice while digging your toes into the sand and listening to waves crash on the beach, ALEX will deliver longer-term benefits (and save your employees money while relieving their stress).


